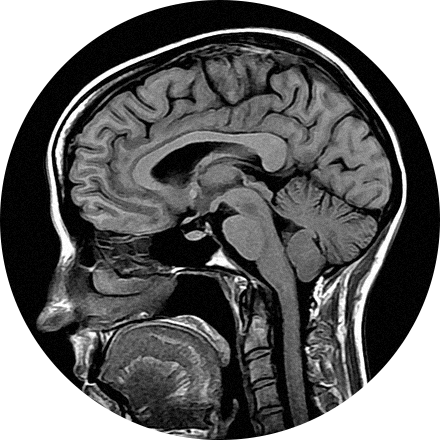
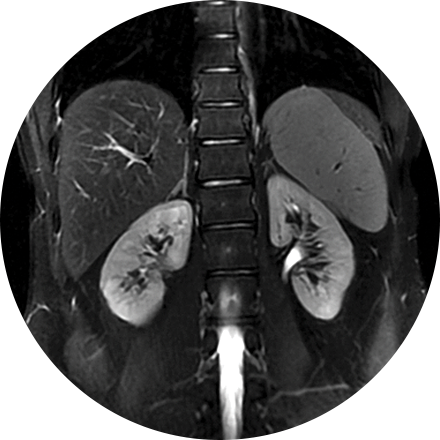
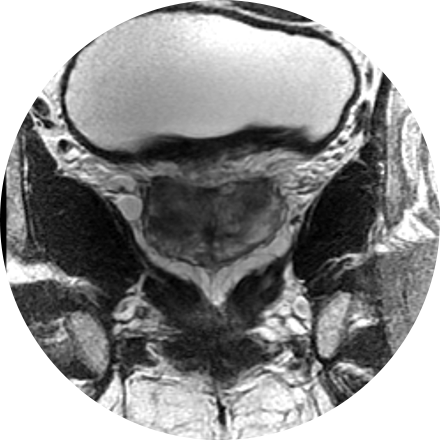
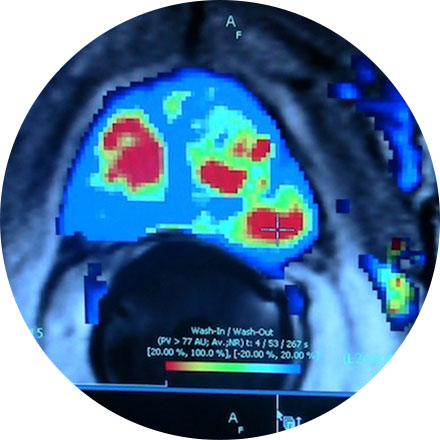
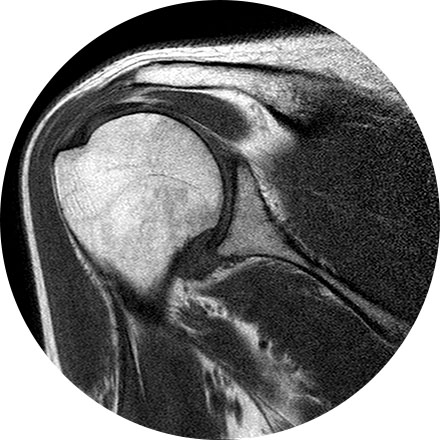
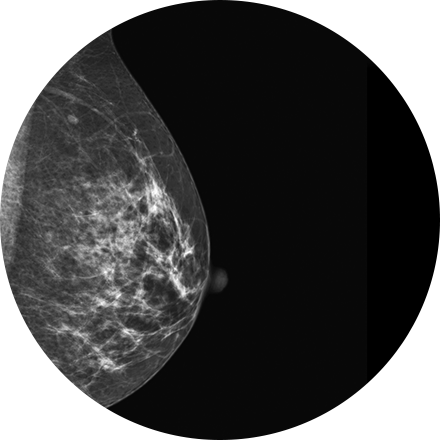
This is considered the standard for state-of-the-art imaging and is ideal for abdomen and chest MRIs.
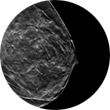
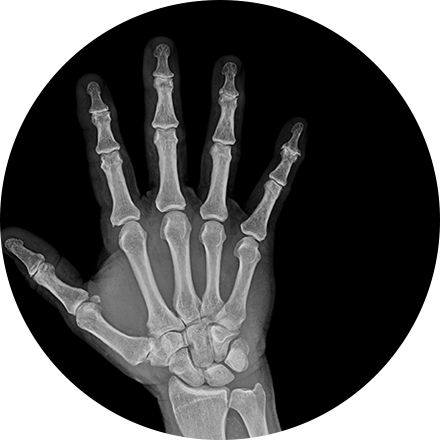
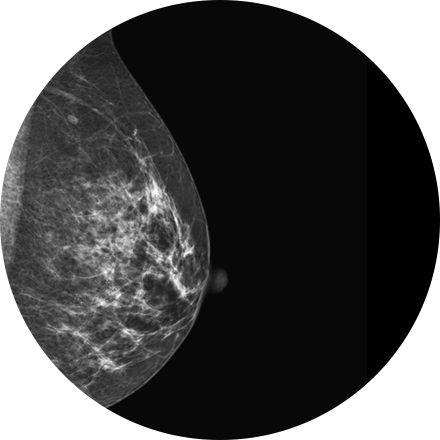
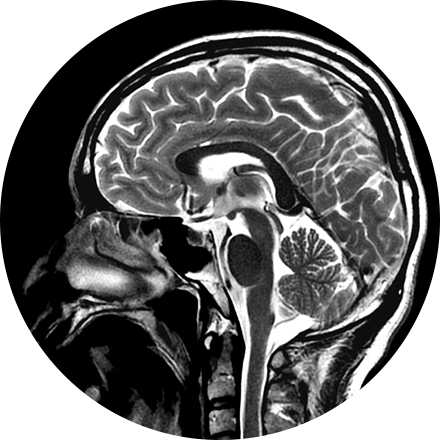
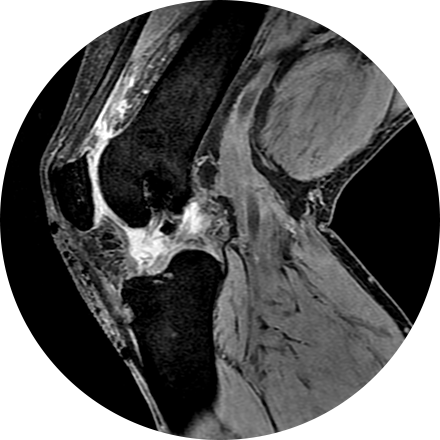
3T MRI uses one of the strongest magnets available to patients and referring physicians to produce medical images. A 3T MRI machine has a more powerful magnet than a 1.5T MRI machine. It is appropriate for detecting many musculoskeletal problems, especially in small joints. It is also useful for evaluating the breast, tiny abnormalities in the brain and spinal cord and some parts of the abdomen and pelvis.
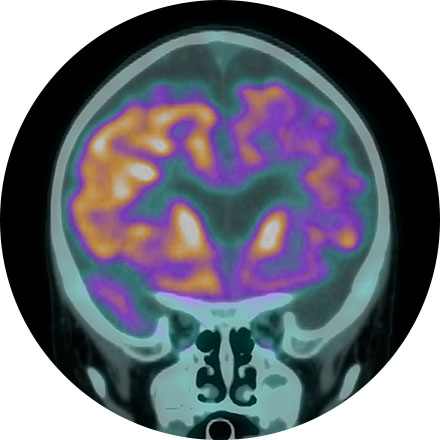
Description for Amyloid Brain Imaging.
Amyloid brain PET/CT is used to directly image amyloid deposition in the brain which can be found in patients with Alzheimer’s Disease. This can help confirm or exclude this diagnosis in patients with memory loss. Amyloid PET can be positive in patients with Alzheimer’s up to 20 years before the patient becomes symptomatic.
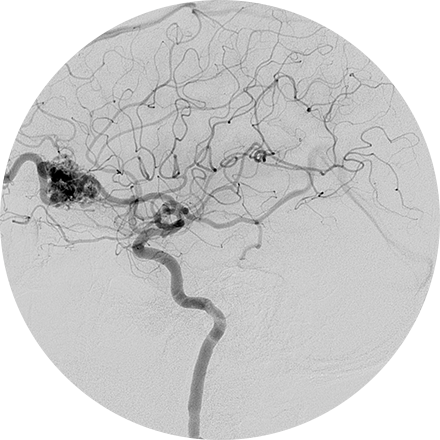
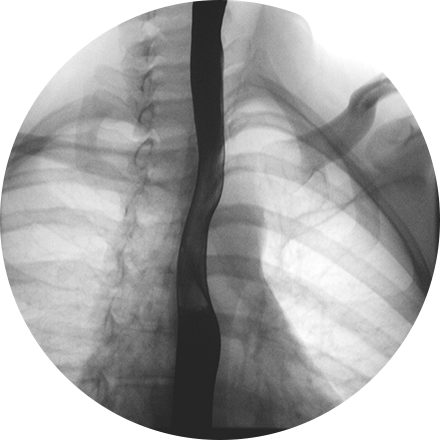
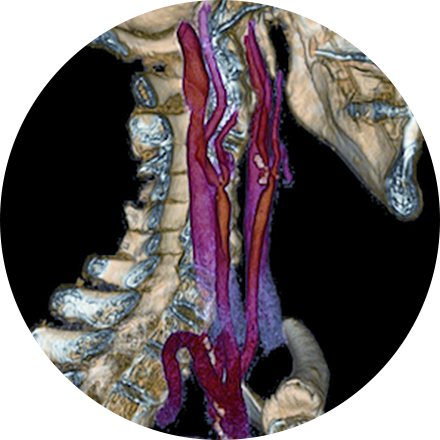
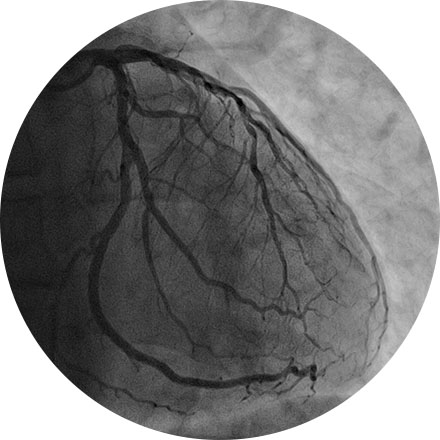
An angiogram is an X-ray exam of the arteries and veins to diagnose blockages and other blood vessel problems. It can reveal the integrity of the cardiovascular system in specific areas throughout the body. Combined with the use of intravenous contrast medium injected via a catheter, an angiogram identifies areas of blockage or damaged vessels within the circulatory system. CT and MRI may also be used to gain additional images of the arteries.
An arthrogram is an X-ray exam of a joint, using a contrast agent and fluoroscopy (a live motion X-Ray). It is used to diagnose the cause of pain or restricted motion of a joint as well as injury to the components of the joint including, the tendons, soft tissues, ligaments, labrum, cartilage and bones. Often this procedure is used to image the shoulder and hip joints, and it is also used when investigating the knees, elbows, ankles and wrists. CT and MRI may also be used to gain additional images of the joint.
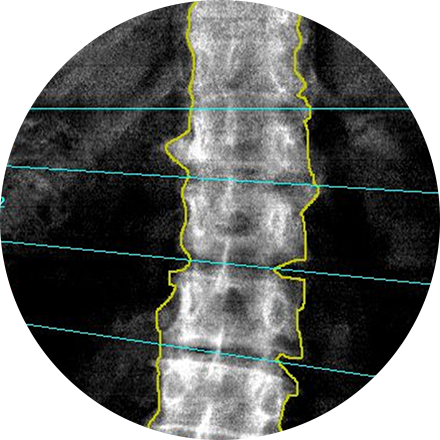
A dual-energy X-ray absorptiometry (DEXA) scan measures the density and mineral content in bone, most often in the hip or lower spine. It is the most accurate method of determining bone density and potential problems related to bone loss. This test is a valuable tool for diagnosing osteoporosis, which often has no symptoms until you suffer a fracture. A bone density scan can diagnose the disease at its earliest stages, which means you can begin receiving treatment to protect your bones sooner.
Your provider may request a breast biopsy if a lump or abnormality is found during screening. A biopsy is a very accurate, minimally invasive method of locating and removing tissue for further investigation. Image-guided biopsy allows patients to avoid hospitalization and general anesthesia (previously necessary with traditional surgical biopsy). It is a valuable method of getting a fast, accurate, conclusive diagnosis—without unnecessary time, pain or expense to the patient.
Depending on your medical needs, we provide different diagnostic biopsy procedures:
Stereotactic biopsy uses mammography to precisely guide clinicians to a lump or abnormality that can’t be felt or seen on ultrasound. Clinicians see a 3D picture of the lump’s exact location.
MRI-guided biopsy uses MRI to guide the radiologist to the exact location of the lump. MRI biopsy is usually used when the lump can be seen on breast MRI, but cannot be readily seen on mammogram or ultrasound.
What happens during a biopsy procedure?
While the biopsy is performed, you will either remain seated in a comfortable, upright position or you will lie face down on a special table that allows your breast to be placed in an opening. The radiologist performs a core needle or vacuum-assisted biopsy (see below) while your breast is somewhat compressed in the mammographic biopsy system. You can return home in 30 minutes.
Vacuum-assisted biopsy devices are used for stereotactic and MRI guided biopsy and selected="selected" ultrasound guided biopsies. The device is a special probe that applies suction and allows retrieval of more tissue. Breast tissue is drawn into the sampling chamber of the probe with the vacuum and then cut. Several pieces of tissue are always obtained during biopsies, regardless of the type of needle used.
In a core needle biopsy, the radiologist locates the lump or abnormality that can be seen on a mammogram, sonogram or MRI. A hollow core needle is then placed inside the abnormality. The needle will then withdraw a small amount of tissue that will be sent to a lab for analysis. Prior to the procedure, you will be given some local anesthetic similar to the anesthetic used for dental procedures to numb the area. You may feel some pressure and mild discomfort but most patients do not feel pain. The doctor will insert the needle several times to get adequate tissue samples. After the procedure, you can resume normal activities immediately. You may experience some slight bruising but should not have a scar. It may take several days to one week to obtain results from the lab.
Some women — because of their family history, a genetic tendency or certain other factors — should be screened with MRI in addition to mammograms. The number of women who fall into this category is small: less than 2 percent of all the women in the United States. Talk with your doctor about your history and whether you should have additional tests.
Breast MRI helps to detect small lesions sometimes missed by mammography — without using radiation or compressing the breasts. MRI uses powerful magnets and radio waves to take very clear pictures of soft tissues, so it can be extremely useful in breast imaging.
Ultrasound uses sound waves instead of X-rays to examine breast tissue. A transducer is passed over the breast. The transmitted sound waves are translated into a picture on a monitor. It does not cause discomfort and, because it does not use radiation, it carries very little risk.
Ultrasound is useful for women with dense breasts or for evaluating suspicious areas seen by mammography or felt during a breast exam. It can also find breast lesions that are close to the chest, where mammography is less useful. Breast ultrasound can distinguish between cysts, which are fluid-filled, versus other types of solid breast masses.
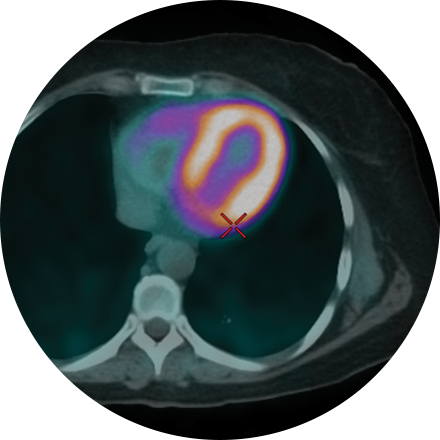
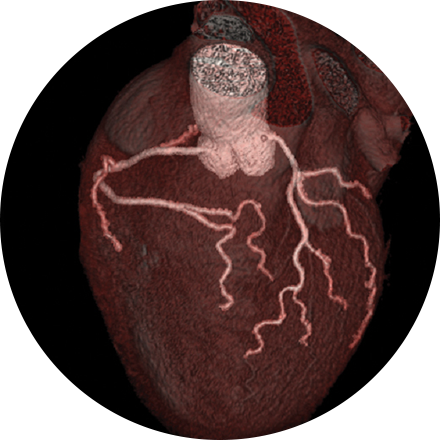
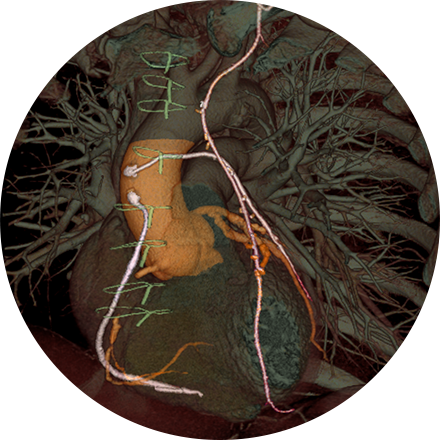
Cardiac MRI is used to obtain detailed images of the heart. It helps physicians evaluate heart structures, such as the cardiac chambers and valves, major vessels and the pericardium (a small structure that surrounds the heart). Disorders such as coronary artery disease, irreversible scarring after a heart attack, tumors, infections, and inflammation can all be diagnosed and monitored using MRI. Physicians also use MRI to plan future patient’s treatment.
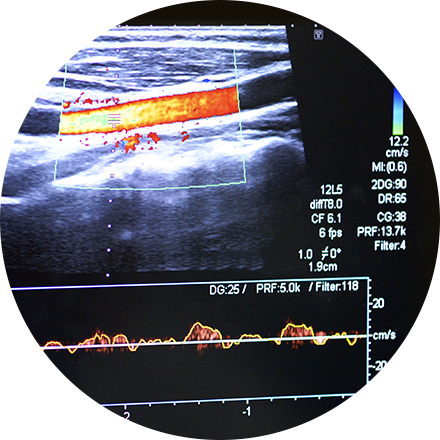
Carotid ultrasound uses sound waves to produce pictures of the carotid arteries in the neck which carry blood from the heart to the brain. A Doppler ultrasound study, a technique that evaluates blood flow through a blood vessel, is usually a part of this exam. It is most frequently used to screen patients for blockage or narrowing of the carotid arteries which may increase the risk of stroke.
A chest X-ray is a very common medical procedure that can reveal the cause of chest pain, persistent cough or difficulty breathing. A very small dose of radiation is used to image the lungs, heart and other structures in the chest.
This exam is part of a sophisticated high-speed CT exam of the heart. During the scan, which takes just seconds, the equipment measures the amount of calcium present and calculates a score. The lower the score, the lower the potential risk of an adverse future cardiac injury. (Calcium often covers the atherosclerotic plaque that builds up inside arteries. This plaque and calcium can lead to narrowing of the inside of the arteries which could in turn lead to an increased risk of angina, and a heart attack.) This test can assess coronary heart disease, which is often asymptomatic and is the most common cause of death for patients in the United States.
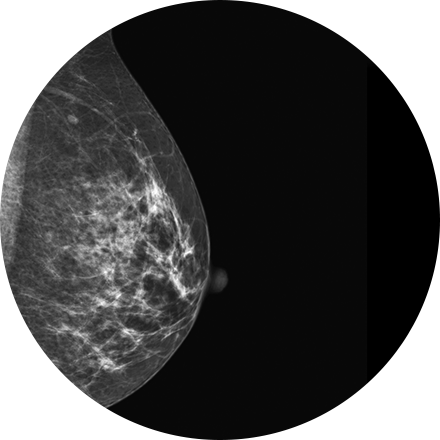
Mammography is a type of low-dose X-ray of the breast. It reveals masses and micro-calcifications within and around the breast that may indicate breast problems including, but not just limited to cancer.
Experts recommend a mammography screening of the breasts at regular intervals to increase the chance of early cancer detection and treatment. The American College of Radiology recommends women aged 40 and older should have a screening mammogram every year and should continue to do so for as long as they are in good health.
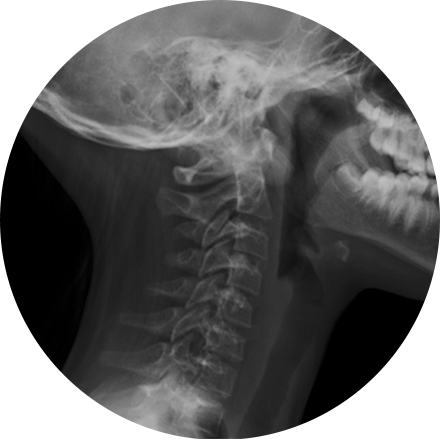
X-ray is the oldest and most economical form of medical imaging. During the procedure, radiation passes through the body onto “film” (now digitized and displayed on a computer screen). In neuroimaging, spinal X-rays are used to assess for the degree of spinal motion with flexion or extension.
This is an accurate and noninvasive imaging procedure used to assess and evaluate certain gastrointestinal problems, such as inflammatory bowel disease (including Crohn’s Disease), infectious enteritis, lymphoma or tuberculosis. It also can be used in patients with gastrointestinal bleeding to determine if a small bowel polyp is causing the bleeding. Enterography may be performed using MRI or CT.
A FDG brain PET/CT is used to image the metabolic function of the brain. Positron emission tomography (PET) uses small amounts of radioactive materials called radiotracers, a special camera, and a computer to help evaluate the brain. It is most commonly used to calculate the degree and pattern of brain volume loss, which allows the neuroradiologist to assess for different types of neurodementia syndromes. It can also help differentiate recurrent brain tumor vs. radiation change after a patient has had brain surgery. Additionally, it can help identify the seizure focus in patients with epilepsy.
The most common organs to be examined using fluoroscopy in children are the gastrointestinal tract (esophagus, stomach, small and large intestines) and the urinary tract (bladder, ureters, urethra). These studies involve contrast and, in some cases, a period of fasting before the exam.
The biliary system is comprised of the liver, gallbladder and bile ducts, and a hepatobiliary exam, or HIDA, evaluates issues in that system. A radioactive tracer is injected (or inhaled or swallowed) and then taken up by the target organs. In this way, the clinician can see how well they function. It shows if the bile ducts are closed or leaking, or if the gallbladder is inflamed, or if the liver is abnormal. HIDA is a nuclear medicine test, which delivers information that often cannot be obtained by other procedures.
3D mammography (tomosynthesis) is an FDA-approved technology that complements conventional 2D mammography. While traditional mammography generates 2D images, 3D mammography creates multiple thin 3D image slices that allow each section of the breast tissue to be seen more clearly.
New imaging software used with our 3D mammogram units enables us to offer a lower-dose 3D exam. The software eliminates the need to obtain additional 2D images as part of the 3D exam, as previously required. This reduces the radiation dose, making it similar to that of a traditional 2D mammogram.
A 3D mammogram looks and feels like a regular mammogram. An x-ray arm scans over your breast taking multiple 3D images at various angles. Each scan takes about 4 seconds and the entire 3D mammogram lasts about 15-20 minutes.
Lung cancer CT screening is one of the most accurate diagnostic tools for finding lung cancer at an early stage, when it is most treatable. CT scans of the lung are able to detect small abnormalities in the lungs that could be the beginning stages of lung cancer. These indicators are often not visible on a routine chest X-ray. Since a CT lung screening offers the best opportunity for successful treatment of lung cancer before symptoms are noticed, more physicians are opting for lung cancer screening based on risk factors (like smoking and family history), rather than symptoms.
A ventilation/perfusion lung scan (also known as a V/Q lung scan) assesses the circulation of air (ventilation) and blood (perfusion) in a patient’s lungs. The exam is useful for identifying blood clots or abnormal flow in the lungs or serious lung disorders such as chronic obstructive pulmonary disease (COPD) or a pulmonary embolism. The V/Q scan uses intravenous material (radiotracers) to show the functional health of the organs.
MRI-guided biopsy uses MRI to guide the radiologist to the exact location of the area of concern. MRI biopsy is usually used when the abnormality can be best seen on breast MRI, but not as well visualized on mammogram or ultrasound. Often lesions that are biopsied are done under the imaging modality that best demonstrates them.
Image-guided biopsy allows patients to avoid hospitalization and general anesthesia (previously necessary with traditional surgical biopsy). It is a valuable method of getting a fast, accurate, conclusive diagnosis—without unnecessary time, pain or expense to the patient.
A multi-gated acquisition (MUGA) scan creates video images that show whether the lower chambers (ventricles) of the heart are pumping blood properly. MUGA uses intravenous material (radiotracers) to show how blood moves through the heart. MUGA can be used to check for pre-existing cardiac conditions prior to chemotherapy, or after treatment to assess possible side effects.
Myelography is an exam in which contrast material is injected into your spinal column and then that contrast and spinal anatomy is imaged with CT technique. This allows the neuroradiologists to evaluate areas of nerve root impingement, canal narrowing, or disc protrusions. It is typically used when a patient is not a candidate for MRI.
This non-invasive exam shows how well blood perfuses (flows through) your heart muscle—in other words, how well your heart is pumping. Sometimes known as a nuclear stress test, it can be performed while the patient exercises on a treadmill or, if that is inadvisable, using a medicine that simulates the effect of exercise on the heart. Myocardial perfusion is an effective way to assess narrowed arteries, the effects of a past heart attack, or the viability of further procedures, such as a stent.
Cardiac nuclear medicine studies help physicians diagnose the cause and exact location of chest pain and visualize blood flow patterns to the heart (myocardial perfusion scan), scan for heart attack damage, assess the heart post-surgery (bypass or re-vascularization), and see the heart-wall movement (in conjunction with an electrocardiogram, or ECG).
A nuclear “stress test” takes images of your heart at rest and after your heart has been “stressed.” The two are compared to reveal if there is any damage to your heart muscle. This procedure helps evaluate coronary artery disease, acute chest pain, hibernating myocardium and cardiomyopathies. Initially, you will be injected with an isotope, and (30 minutes later) resting images will be acquired. The stress portion is next, which involves either a treadmill or injection of medications that mimic physiological stress. A second isotope is injected for this portion of the test. After your heart rate returns to normal and you eat, the technologist takes the final set of images of your heart.
One of the more frequent applications of ultrasound is in the evaluation of a fetus. Most obstetricians perform a routine diagnostic ultrasound to look for any abnormalities with either the fetus or the mother’s anatomy during early pregnancy. Depending on the time of gestation and positioning, the gender may or may not be identified. This ultrasound procedure is painless and non-invasive.
Ultrasound imaging of the pelvis uses sound waves to produce pictures of the structures and organs in the lower abdomen and pelvis. There are various types of pelvic ultrasound including abdominal, vaginal and rectal. These exams are frequently used to evaluate the reproductive and urinary systems. Ultrasound is safe, noninvasive and does not use ionizing radiation.
Prostate imaging focuses on three major health problems centered on the prostate gland: cancer, benign enlargement and inflammation (the cause of most urinary tract infections). Radiology plays an important role in diagnosing and treating these problems. For more information about our Prostate MRI Program please visit mriprostatecancer.com.
Magnetic resonance imaging (MRI) of the prostate uses a powerful magnetic field, radio waves and a computer to produce detailed pictures of the structures within a man’s prostate gland. It is primarily used to evaluate the extent of prostate cancer and determine whether it has spread. It also may be used to help diagnose infection, benign prostatic hyperplasia (BPH) or congenital abnormalities.
Description for Renal Scan.
A renal ultrasound is a safe and painless test that uses sound wavesto produce images of the kidneys and bladder. The kidneys are a pair of bean-shaped organs located toward the back of the abdominal cavity, just above the waist. They remove waste products from the blood and produce urine.
Ultrasound imaging of the scrotum uses sound waves to produce an image of a man’s testicles and the surrounding tissue. It is primarily used to help evaluate disorders of the testicles, and scrotum. Ultrasound does not use ionizing radiation.
CT of the sinuses uses special x-ray equipment to evaluate the hollow, air-filled spaces within the bones of the face surrounding the nasal cavity. CT scanning is painless, noninvasive and accurate. It’s also the most reliable imaging technique for determining if the sinuses are obstructed and the best imaging modality for sinusitis.
Positron emission tomography (PET) and computed tomography (CT) are state-of-the-art diagnostic imaging tools. A PET/CT scan with a sodium fluoride injection is an imaging test that scans the entire skeletal system and produces images of the bones. These images are used to detect areas of abnormal bone growth associated with tumors that may have spread from different parts of the body.
Stereotactic biopsy uses mammography to precisely guide clinicians to a lump or abnormality such as an area of calcification, that cannot be felt or seen on ultrasound. Clinicians see a 3D picture of the lump’s exact location.
Image-guided biopsy allows patients to avoid hospitalization and general anesthesia (previously necessary with traditional surgical biopsy). It is a valuable method of getting a fast, accurate, conclusive diagnosis—without unnecessary time, pain or expense to the patient.
A three phase bone scan is a nuclear medicine test that uses radiotracers, which are injected. The radiotracers are detected by a special camera to provide pictures to diagnose a fracture when it cannot be seen on an X-Ray. It is also used to diagnose bone infection, bone pain, osteomyelitis, and other bone diseases.
A thyroid scan shows, in video images, how well a patient’s thyroid is functioning, along with its structure and position. This type of study can be used to diagnose hyperthyroidism, cancer, and other abnormalities, such as lumps or inflammation, in this important organ. Like other scans that are used to determine whether an organ is functioning properly, a thyroid scan is a nuclear medicine test; that is, it uses intravenous radiotracers detected by a special camera to provide pictures that show
Thyroid ultrasound uses sound waves to produce images of the thyroid gland in the neck. This procedure is typically used to evaluate lumps (or nodules) found during a routine physical and to determine if they are the more common benign nodule or if they have features that require a biopsy. Ultrasound does not use ionizing radiation.
Transvaginal ultrasound imaging of the abdomen uses sound waves to produce pictures of the structures and organs in and around a woman’s uterus. Transvaginal (TV) ultrasounds are performed very much like a gynecologic exam and involves the insertion of an ultrasound transducer into the vagina to study the lining of the uterus. These exams are frequently used to evaluate the reproductive and urinary systems. Ultrasound is safe, noninvasive and does not use ionizing radiation.
Vascular ultrasound uses sound waves to image the body’s veins and arteries. A special ultrasound technique, called Doppler, evaluates blood flow through vessels in the abdomen, arms, legs, neck and head. It helps the physician find tumors, congenital malformations, narrowing (as with plaque accumulation), and blocks (as with deep-vein thrombosis). It also helps clinicians assess the health of the arteries before or after a procedure, i.e., to judge whether an angioplasty is advisable or if a graft is succeeding.
This exam is most commonly used for diagnosing metastatic disease or primary bone cancers. It may also be used to diagnose Paget’s disease, fractures (old vs. new or post trauma), unexplained bone pain, and other bony abnormalitites.
The procedure itself is non-invasive and simple. The patient receives an intravenous injection of a radiotracer. There are virtually no side effects or allergic reactions to this or any other radiopharmaceutical. The patient may leave after injection and return approximately 3 hours later for the scan. You’ll be asked to lie still on a table while an armlike device supporting a tracer-sensitive camera passes back and forth over your body. Patients are encouraged to stay well hydrated to improve the images. Otherwise they may resume their normal routine. The whole body bone scan takes approximately 45 minutes to one hour for most patients.
Because the radiation dose comes from the injection not the camera, additional images may be obtained of any area of interest, sites of pain, etc. without additional exposure for the patient.
A whole body scan can be appropriate for a high-risk patient with a history of heart disease, cancer, smoking, hypertension, or diabetes, or one who has been exposed to hazardous chemicals. The prime benefit of whole body scanning is the ability to locate and diagnose a disease process that can be effectively treated if found early, such as gall stones, degenerative and arthritic changes of the spine, kidney stones, abnormal lymph nodes and many other issues. Logistics are similar to the standard CT discussed on this page.